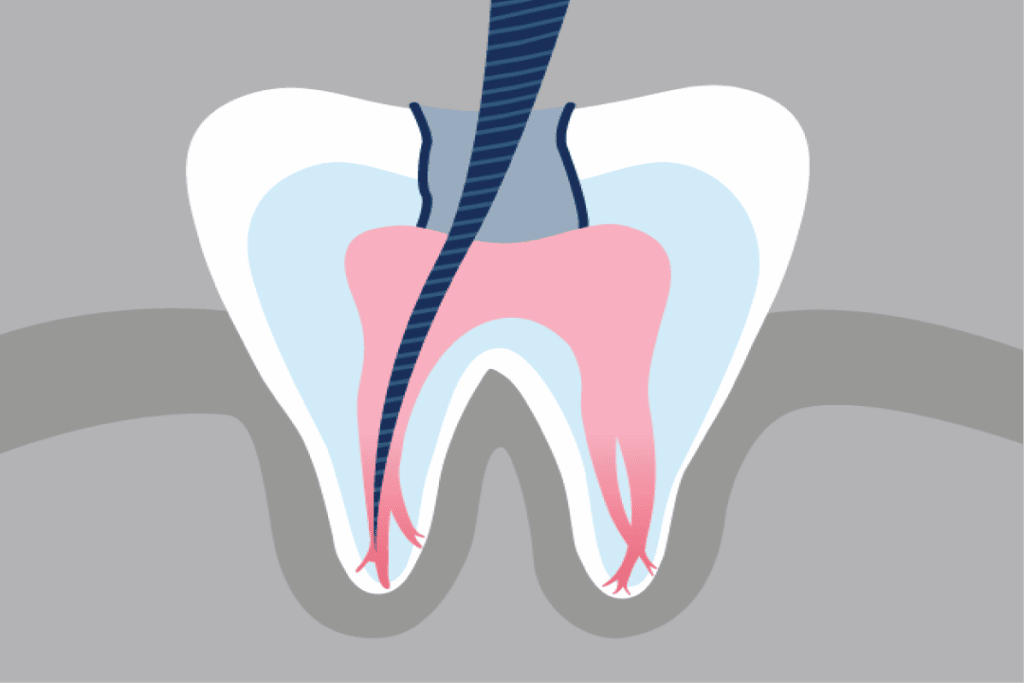
Why a Root Canal is Rarely Optional
Root canals are necessary in instances where the tissues, nerves, and blood vessels inside the tooth–called the dental pulp–have become infected and can’t be treated with a filling like a small cavity can. During the procedure, the dentist drills a hole into the affected tooth, cleans out the inside of all infected tissue, and fills the tooth with a material called gutta percha, which is strong and acts like natural tooth material.
While not all toothaches will require a root canal, a root canal is typically the only option for a tooth with infected dental pulp, because an infected tooth will not heal. If left untreated, the infection in the pulp will create an abscess, or pus pocket, that will eventually erode and compromise the tooth roots, making the tooth less stable and more challenging to save. Without the root canal, the bacteria from the infection will also spread to other tissues in the gum and mouth as well as the jaw bone, blood, or even the brain, leading to tooth loss, bone deterioration, or more serious health concerns.
Only a dentist can determine whether or not you need a root canal, but there are several signs that could indicate inflammation or an infection, such as:
- Pain localized to one specific tooth
- Swollen gums around the tooth
- Gums that are red or tender to the touch
- Facial swelling
- A tooth that changes color, usually becoming darker
- A visible hole or chip in the tooth
- A pimple-looking bump on the gums near the tooth
- Pain when eating or drinking that doesn’t stop as soon as the hot or cold food is removed
Anyone might need a root canal—even children who haven’t grown in their adult teeth yet—but this procedure is most commonly done on people between the ages of 33 to 44.